Transdermal patches offer a convenient way to deliver medications through the skin, a method widely referred to as transdermal patches. By releasing active ingredients steadily, they promote predictable blood levels, improve adherence, and reduce first-pass metabolism. In this guide you will learn about types of transdermal patches, common transdermal patch uses, and essential transdermal patch safety tips. We also explain how transdermal patches work and why transdermal drug delivery can be advantageous for certain therapies. Whether you are curious about nicotine patches, pain relief formulations, or hormonal therapies, understanding these systems can help you make informed treatment decisions.
Framed in alternative terminology, these skin based delivery systems place a medicated patch on the body to release medicine over time. Researchers describe them as percutaneous or transcutaneous adhesive drug delivery methods that bypass the gut and liver on first pass. Other terms include topical drug delivery patches, adhesive reservoirs, and drug in adhesive configurations that achieve steady systemic exposure. LSI inspired explanations highlight how such systems use controlled release, skin diffusion, and compatibility with patient lifestyles to support adherence. By exploring these related concepts, readers gain a clearer sense of the options, safety considerations, and clinical contexts in which skin based therapy may be preferred.
How Transdermal Patches Work: From Skin to Systemic Delivery
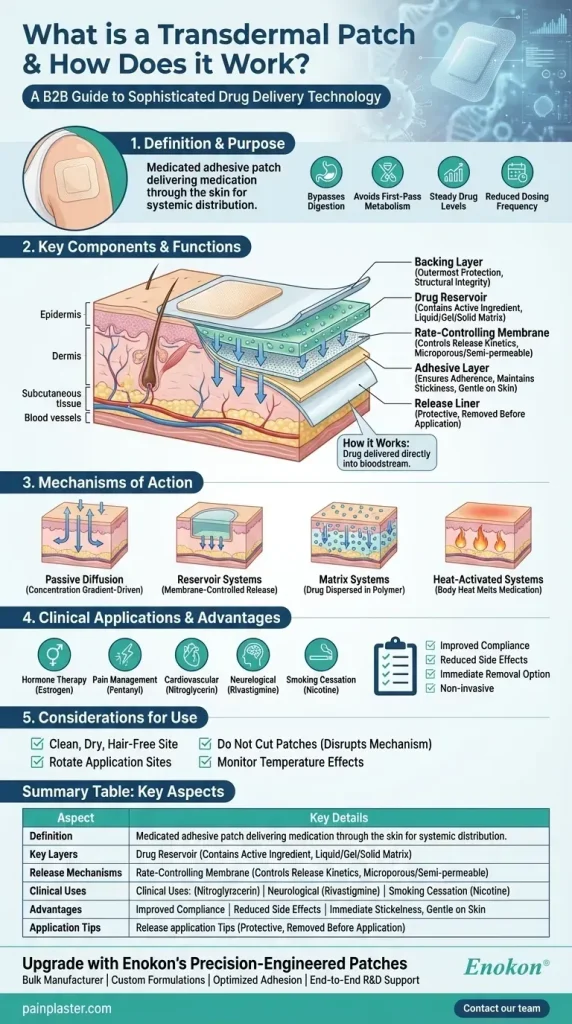
Transdermal patches deliver medication by embedding the active drug in an adhesive matrix or reservoir and placing it on the skin. From there, the drug diffuses through the outer skin layer (the stratum corneum) and into the bloodstream, bypassing the digestive system and its first-pass metabolism in the liver. This mechanism supports a steady, controlled release of medication over a specified wear time.
The effectiveness of this delivery depends on the drug’s properties—such as lipophilicity and molecular size—as well as the patch design, site of application, and skin condition. Proper preparation of clean, dry skin and correct placement are essential to achieving predictable blood levels and minimizing variability between wear cycles.
Types of Transdermal Patches: Reservoir, Matrix, Drug-in-adhesive, and Iontophoretic Designs
Transdermal patches come in several core designs. Reservoir patches contain a drug solution in a separate compartment beneath an adhesive layer, with a rate-controlling membrane that modulates release. Matrix patches embed the drug within a solid or semi-solid matrix that doubles as the adhesive, allowing the medicine to migrate out over time.
Drug-in-adhesive patches disperse the active drug directly within the adhesive itself, simplifying construction and often reducing patch size. Advanced iontophoretic and other electrically assisted patches use a small current to drive charged molecules through the skin, illustrating ongoing innovation in transdermal drug delivery.
Transdermal Patch Uses: From Nicotine to Hormonal Therapies
One of the best-known transdermal patch uses is nicotine patches for smoking cessation, delivering nicotine steadily to lessen withdrawal symptoms and support behavioral change. This application highlights how steady dosing can improve adherence and outcome without pills.
Beyond nicotine, fentanyl patches provide long-acting analgesia for chronic, severe pain when other methods are insufficient. Hormonal patches for estrogen, progestin, or contraception address menopausal symptoms and family planning needs, while patches for motion sickness (scopolamine) and localized pain relief (lidocaine) demonstrate the versatility of transdermal delivery across therapeutic areas.
Safety Considerations and Potential Side Effects of Patches
Transdermal patch safety includes monitoring for skin reactions such as redness, itching, or dermatitis at the application site. If irritation persists, reassessing patch use or trying an alternative delivery method may be necessary to avoid compromising treatment.
Other safety considerations involve dose exposure and heat effects. External heat sources can increase absorption and drug exposure, while interactions with other medications or certain medical conditions may alter risk. Proper disposal of used patches and following clinician guidance are essential for safe practice.
Practical Tips for Applying and Managing Transdermal Patches
To maximize benefits and minimize risks, follow the dosing schedule and apply patches to clean, dry skin on approved sites. Rotate application areas to reduce dermatitis, avoid damaged skin, and ensure you do not cut patches unless explicitly advised by a clinician, as this can alter dosing.
Additional practical steps include removing patches if they become loose, not applying creams or oils under the patch, and storing them away from heat and moisture. If a patch falls off, replace it with a fresh one and seek medical guidance on retiming dosing to prevent gaps in therapy.
The Future of Transdermal Patch Technology and Drug Delivery
Researchers are advancing transdermal patch technology to broaden safety, efficacy, and patient comfort. Developments include improved skin-friendly adhesives, more precise rate-controlling membranes, and patches designed for a wider range of drugs, including complex molecules.
Innovations such as microarray and microneedle-assisted patches aim to expand transdermal drug delivery to molecules previously challenging to administer through the skin. These advancements support the ongoing evolution of transdermal drug delivery, potentially enabling broader use, better adherence, and new therapeutic possibilities.
Frequently Asked Questions
What are the main types of transdermal patches and how do they differ?
Transdermal patches come in several designs, including reservoir patches, matrix patches, drug-in-adhesive patches, and iontophoretic (advanced) patches. Reservoir patches contain a liquid or gel drug solution with a rate‑controlling layer for precise release; matrix patches embed the drug in a solid or semi‑solid matrix; drug‑in‑adhesive patches disperse the drug directly within the adhesive; iontophoretic patches use electricity or other methods to boost delivery. These designs influence release rates, patch size, and suitability for different drugs and patients.
How do transdermal patches work to deliver drugs through the skin?
Transdermal patches solubilize the active drug in the patch and rely on controlled diffusion through the skin layers, starting with the outer stratum corneum and reaching deeper tissues and blood vessels. This mechanism provides a steady release over hours to days and helps avoid first‑pass liver metabolism, contributing to more predictable blood levels.
What are common uses of transdermal patches?
Common uses of transdermal patches include nicotine patches for smoking cessation, fentanyl patches for chronic pain, hormonal patches for menopause or contraception, scopolamine patches for motion sickness, and lidocaine patches for localized pain. The choice depends on pharmacokinetic needs and patient preferences for ease of use and avoiding pills.
What safety considerations should be noted with transdermal patches?
Key safety concerns include skin reactions at the application site, potential for increased absorption with external heat, and adherence to prescribed wear time. Also consider potential drug interactions, medical history, and avoiding damaged skin, proper disposal of used patches, and consulting a healthcare provider if adverse effects occur.
Who should approach caution or supervision with transdermal patches?
Transdermal patches may not be suitable for everyone. People with adhesive allergies, certain skin conditions, pregnancy or breastfeeding, or specific medical contraindications should use patch therapies under medical supervision. Pediatric dosing requires clinician input to ensure safety and efficacy.
What practical tips help ensure effective use of transdermal patches?
Tips include applying to clean, dry skin on approved sites, rotating sites to minimize irritation, avoiding creams or powders under the patch, not cutting patches unless directed, monitoring wear time, and storing patches as directed away from heat and moisture. If a patch falls off, follow clinician guidance for resuming dosing.
| Aspect | Key Points |
|---|---|
| Definition / What they are | An adhesive patch worn on the skin that releases a predefined drug dose over a period; bypasses the digestive system and first-pass liver metabolism; provides more predictable blood levels than some oral medications. |
| How they work | Active drug is solubilized in the patch’s matrix or reservoir and diffuses through the skin’s outer layer into deeper tissues and the bloodstream, providing a steady release rate. Effectiveness depends on drug properties (lipophilicity, size), patch design, skin condition, and application site. Proper skin preparation and placement are essential for consistent results. |
| Advantages | – Steady drug delivery over hours to days, reducing the need for multiple daily doses – Improved convenience and adherence for chronic conditions – Avoidance of gastrointestinal side effects for some medicines – Potentially improved tolerability for drugs with poor oral bioavailability |
| Reservoir patches | Contain a liquid or gel-like drug solution in a separate reservoir beneath the adhesive; drug diffuses through a rate-controlling membrane or the adhesive; offers precise control but can be more complex to manufacture. |
| Matrix patches | Drug is within a solid or semi-solid matrix that also forms the adhesive layer; drug migrates out of the matrix into the skin over time; simple, reliable, and versatile release rates. |
| Drug-in-adhesive patches | Drug dispersed directly within the adhesive, eliminating a separate drug-containing layer; patch tends to be smaller, lighter, and easier to customize for dosing. |
| Iontophoretic and advanced patches | Use electrical current or other physical means to enhance drug delivery; iontophoretic patches apply a small current to drive charged drugs into the bloodstream; not as common as nicotine or fentanyl patches, but illustrate ongoing innovation. |
| Common uses and examples | Nicotine patches for smoking cessation; Fentanyl patches for chronic pain; Hormonal patches (estrogen, progestin); Scopolamine patches for motion sickness; Lidocaine patches for localized pain relief; other analgesic or cardiovascular agents suited to steady dosing or avoidance of first-pass metabolism. |
| Safety considerations | – Skin reactions: redness, itching, dermatitis; assess persistence or worsening – Dose/exposure: higher-dose patches or long wear increase risk of systemic side effects if damaged or worn longer than prescribed – Heat and absorption: external heat sources can increase patch absorption – Interactions and medical history: drug interactions and contraindications; evaluate risk with clinician – Skin integrity: damaged or irritated skin affects performance – Disposal and handling: used patches may still contain drug; fold adhesive sides and dispose safely away from children |
| Practical tips for use | – Read patient information leaflet and follow instructions – Apply to clean, dry, flat skin on approved site; rotate sites – Check wear time and replace on schedule; do not exceed duration – If patch falls off, reapply a new one or consult clinician – Do not apply creams/oils/powders under patch; affect adhesion – Store patches per directions away from heat/moisture |
| When not to use | – Adhesive allergies or skin conditions; contraindications may require alternative delivery – Pregnant or breastfeeding; use under medical supervision – Pediatric considerations; dosing requires clinician input |
| Future directions | – Ongoing development of skin-friendly adhesives and improved rate-controlling membranes – Patches for biologics and peptides; broader drug range – Microarray and microneedle-assisted patches to expand delivery with comfort and adherence |
Summary
Transdermal patches offer a versatile and convenient approach to delivering medications, making it easier for patients to manage treatment with steady, predictable drug levels. This descriptive conclusion highlights how transdermal patches bypass the digestive system, reduce first-pass metabolism, and support adherence, while noting considerations around patch design, safety, and future innovations that may expand the range of drugs that can be delivered through the skin. By understanding patch types, usage tips, safety measures, and the evolving technology, patients and clinicians can make informed decisions about transdermal patch therapy and its role in managing pain, menopause symptoms, and other conditions.