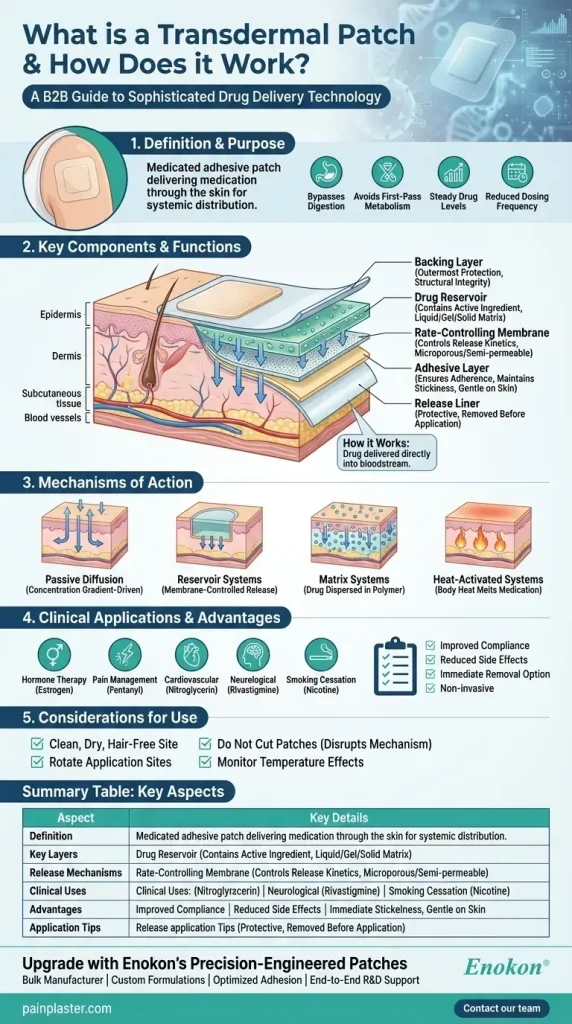
Transdermal patches offer a discreet, controlled-release method for delivering medications through the skin. Many readers want to know how transdermal patches work, and the answer lies in skin biology and patch design. These systems highlight the transdermal patch benefits by delivering a steady drug level and bypassing the digestive tract. There are various types of transdermal patches, each optimized for different drugs and dosing needs. As a skin patch medication approach, it can improve adherence and fit more easily into daily life for patients and caregivers.
From a semantic standpoint, this concept maps to cutaneous drug delivery, skin-mounted therapies, and percutaneous administration. In practice, clinicians consider adhesive patches, drug reservoirs, and rate-controlling mechanisms as ways to achieve steady release through the skin. This broader vocabulary—topical delivery, transcutaneous administration, and wearable patch technologies—helps explain how the same idea fits into different medical contexts.
Introduction to Transdermal Patches and Skin Patch Medication
Transdermal patches are a form of skin patch medication designed to deliver drugs through the skin, providing a controlled release over time. The basic patch design includes a backing layer, a drug reservoir or matrix, an adhesive, and a release-rate element that shapes how the medicine enters the body.
This delivery approach offers practical benefits for patients and clinicians, combining convenience with a predictable pharmacokinetic profile and avoiding some gastrointestinal issues associated with oral dosing. Understanding these features helps explain why transdermal patches are becoming a mainstay in modern pharmacology.
How Transdermal Patches Work: The Delivery Mechanism of Transdermal Patches
In exploring how transdermal patches work, the delivery mechanism of transdermal patches relies on a carefully layered geometry: a protective backing, a drug reservoir or matrix, an adhesive, and a rate-controlling layer. Together, these layers regulate how quickly the active medicine becomes available to the body.
The active agent then crosses the skin’s outer barrier, the stratum corneum, through diffusion aided by formulation strategies such as permeation enhancers and lipid-soluble drugs. This explanation of how transdermal patches work supports a steady plasma concentration and minimizes sharp peaks typical of some oral therapies.
Transdermal Patch Benefits: Why This Delivery Method Is Gaining Ground
Transdermal patch benefits include maintaining steady drug levels, by delivering the medication at a predictable rate and avoiding gastrointestinal fluctuations. This is particularly important for drugs with narrow therapeutic windows, where consistent exposure matters.
In addition, bypassing the GI tract can improve tolerance, facilitate adherence with once-daily or weekly schedules, and reduce dosing burdens for patients who have difficulty swallowing or experience vomiting. This overview highlights the practical value of skin patch medication in daily care.
Types of Transdermal Patches: From Drug-In-Adhesive to Microneedle Systems
Types of transdermal patches cover a range of designs, including drug-in-adhesive patches where the medication is integrated into the adhesive layer, matrix patches with drug dispersed in a polymer matrix, and reservoir patches with a separate drug reservoir.
Emerging formats such as iontophoretic, microneedle, or smart patches use electrical current or tiny penetrators to improve delivery and personalize dosing. These options broaden the toolbox for clinicians and patients alike.
Safety, Dosing, and Real-World Use of Skin Patch Medication
Skin patch medication requires careful attention to safety, dosing, and site selection. Common considerations include skin irritation at the application site, the need to rotate sites, and ensuring wear-time aligns with the prescribed schedule.
Healthcare providers and patients should monitor for systemic effects or interactions with other drugs, and follow labeling guidance on dosing and duration of use. When in doubt, consult a clinician to optimize patch therapy for individual conditions.
The Future of Transdermal Patches: Wearables, Smart Patches, and Personalized Delivery
The future of transdermal patches points toward wearable technologies and smart patches that monitor physiological signals and adjust dosing in real time. Multi-agent patches could deliver combinations of drugs for complex conditions without increasing pill burden.
Ongoing research in materials science, adhesion, and skin compatibility aims to extend wear time, improve comfort, and broaden the range of medicines suitable for transdermal delivery, reinforcing the role of skin patch medication in chronic disease management.
Frequently Asked Questions
How do transdermal patches work, and what is the delivery mechanism of transdermal patches?
Transdermal patches deliver medicine through the skin using layered components—a backing layer, a drug reservoir or matrix, an adhesive, and a rate‑controlling layer. The active drug diffuses across the stratum corneum into underlying tissues and the bloodstream, producing a steady, predictable plasma concentration and smoother therapeutic effect.
What are the transdermal patch benefits?
Key transdermal patch benefits include steady drug levels, avoidance of the gastrointestinal tract, improved adherence, and convenient, once-daily or weekly dosing that fits into daily life.
What are the types of transdermal patches?
Common types of transdermal patches include drug-in-adhesive patches, matrix patches, reservoir patches, iontophoretic patches, and microneedle or smart patches. Each type uses a different release mechanism to suit the drug and patient needs.
What is skin patch medication, and when is it used?
Skin patch medication refers to drugs delivered through patches applied to the skin. It is used for nicotine replacement, hormone therapy, pain relief, motion sickness prevention, and other conditions where steady dosing and avoidance of the GI tract are advantageous.
What factors influence the delivery mechanism of transdermal patches and their effectiveness?
Influencing factors include the drug’s molecular size and lipid solubility, required dose, duration of therapy, and skin condition. Patch design, wear time, and the chosen delivery mode (e.g., passive diffusion vs iontophoretic delivery) also affect how much drug enters the bloodstream and the overall effectiveness.
What safety considerations apply to transdermal patches and to their delivery mechanism of transdermal patches?
Follow the label for dosing and wear time, rotate application sites, and monitor for skin irritation or blistering. Be aware of potential systemic effects or drug interactions, and discuss allergies or skin conditions with a clinician to ensure safe use.
| Aspect | Key Points |
|---|---|
| What are transdermal patches? |
|
| How they work |
|
| Benefits |
|
| Safety and considerations |
|
| Types |
|
| Common medications |
|
| Factors influencing efficacy |
|
| Practical considerations |
|
| Regulatory context |
|
| Future directions |
|
Summary
Transdermal patches represent a significant approach in drug delivery, offering a controlled and convenient way to administer medications through the skin. This overview summarizes how patches work, their key benefits, common types, safety considerations, and future directions. By delivering drugs steadily and bypassing the gastrointestinal tract, transdermal patches can improve adherence and patient comfort across a range of therapies. Choosing the right patch involves considering drug properties, dose and duration, skin condition, and the desired wear time. Safety focuses on proper application, site rotation, and monitoring for irritation or systemic effects. Ongoing research aims to expand the range of drugs suitable for patches, develop multi-agent and smart patches, and enhance materials for comfort and reliability. As technology evolves, transdermal patches are likely to play an increasingly important role in chronic disease management, pain control, and hormone therapy, offering patients a flexible and user-friendly treatment option.